Different viruses cause rubella and rubeola. Rubella is more commonly known as German measles, and people typically refer to rubeola as measles. They can be difficult to tell apart because they have similar symptoms.
Rubella tends to be mild, but it can be dangerous for pregnant people, as the virus may affect a developing fetus or increase the risk of miscarriage. Rubeola is also often mild but can cause serious complications in young children, as it increases their risk of developing pneumonia and encephalitis, which is inflammation of the brain.
There is no specific treatment for rubella and rubeola. Instead, doctors aim to manage symptoms.
People can significantly lower the risk of rubella and rubeola infection by getting the measles, mumps, and rubella (MMR) vaccine.
Read on to learn more about rubella and rubeola.
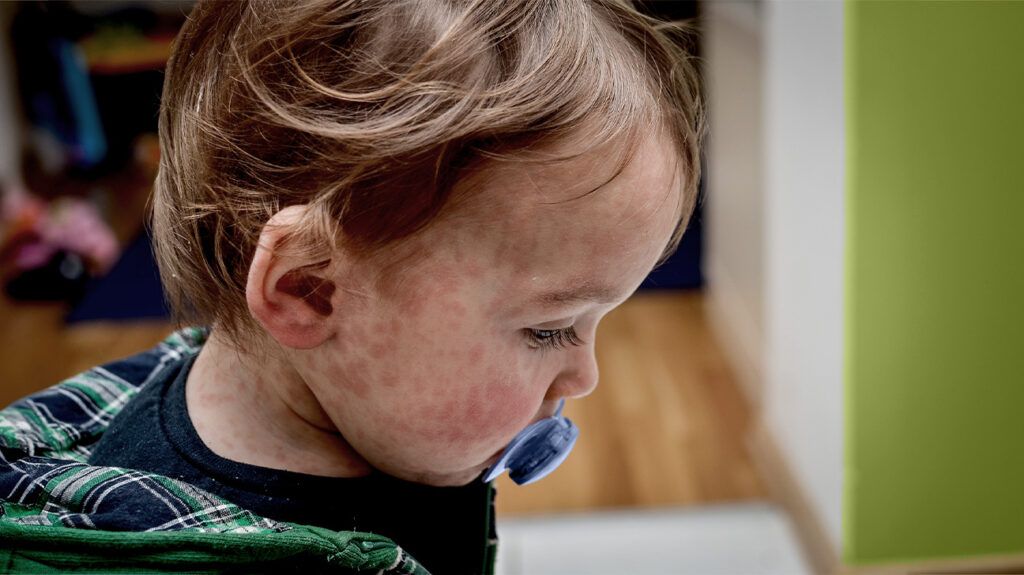
Rubella and rubeola are infectious diseases resulting from different viruses.
According to the
The CDC state that the U.S. eliminated rubeola
People should note that they can still contract rubella and rubeola in the U.S.
Symptoms of rubella and rubeola are similar. However, there are some key differences.
Rubella
Rubella symptoms tend to be mild. Some of the most common symptoms are:
- red or discolored rash on the face that spreads to the rest of the body
- low-grade fever
- sore throat
Rubeola
When a person has contracted rubeola, symptoms tend to appear
- runny or dripping nose
- high fever
- rash
- cough
- conjunctivitis
Most people who contract rubella or rubeola make a swift recovery, but there can be complications.
Rubella
If a pregnant person contracts the virus, the developing fetus they are carrying
- deafness
- cataracts
- heart defects
- developmental problems
- liver and spleen damage
Rubeola
Sometimes, people develop complications after contracting rubeola,
- pneumonia
- encephalitis
- middle ear infection
- croup
- diarrhea due to secondary infections
If pregnant people contract measles, it can be life threatening. If children are
Doctors diagnose rubella and rubeola using a range of tests.
Rubella
A doctor cannot diagnose rubella from a rash alone and would need to use
If a doctor suspects a newborn has contracted rubella in the womb or shortly after birth, they
Doctors typically take several samples, which may include:
- nasopharyngeal swabs
- throat swabs
- urine samples
- blood and serum samples
Rubeola
To confirm a diagnosis of rubeola, a doctor
A healthcare professional may also order a blood count to screen for a decreased platelet and white blood cell count. Additionally, if a person has diarrhea, a doctor may check their electrolyte levels due to a risk of dehydration.
There is no antiviral treatment for rubella and rubeola, and the doctor’s aim is to manage symptoms.
Doctors
Healthcare professionals
Doctors will closely monitor pregnant people with either condition.
Health organizations recommend healthcare professionals administer
According to the CDC, children should receive their first dose of the MMR vaccine between the ages of
In some cases, such as if an infant is traveling out of the country, a healthcare professional may administer the MMR vaccine at an earlier age. A person should discuss their child’s travel vaccinations with a pediatrician.
People can also receive the MMR vaccine in adulthood or adolescence if they did not receive it as a child.
The MMR vaccine and misinformation
People should note that the MMR vaccine
Despite the fact that many subsequent studies have debunked the discredited and withdrawn 1998 article that linked the MMR vaccine to ASD, vaccination rates have declined in the U.S. and United Kingdom.
Anyone who feels hesitant about themselves or a child in their care receiving the MMR vaccine should speak with a healthcare professional who can answer any questions they have.
Viruses cause both rubella and rubeola.
Symptoms of rubella and rubeola are similar, including rashes and fever. There is no antiviral treatment for rubella and rubeola, so doctors can only manage symptoms.
Rubeola can cause serious complications in young children and pregnant people. Similarly, rubella can cause miscarriage and developmental problems in fetuses. Therefore, the CDC recommend that people
A person should seek medical attention if they think they are experiencing symptoms of either condition. Additionally, they should speak with a doctor for further information if they are hesitant about themselves or a child in their care receiving the MMR vaccine.
