Phlebitis and infiltration are complications due to intravenous (IV) therapy. They can cause swelling, pain, and changes in the skin around the IV insertion site. Treatment typically resolves symptoms and prevents complications.
Phlebitis is inflammation of a vein, and infiltration is the leakage of intravenous (IV) fluids or medications into surrounding areas. Both can occur as a complication of having a catheter inserted into a vein.
This article looks at the symptoms, treatment, prevention, and outlook for people with phlebitis and infiltration.
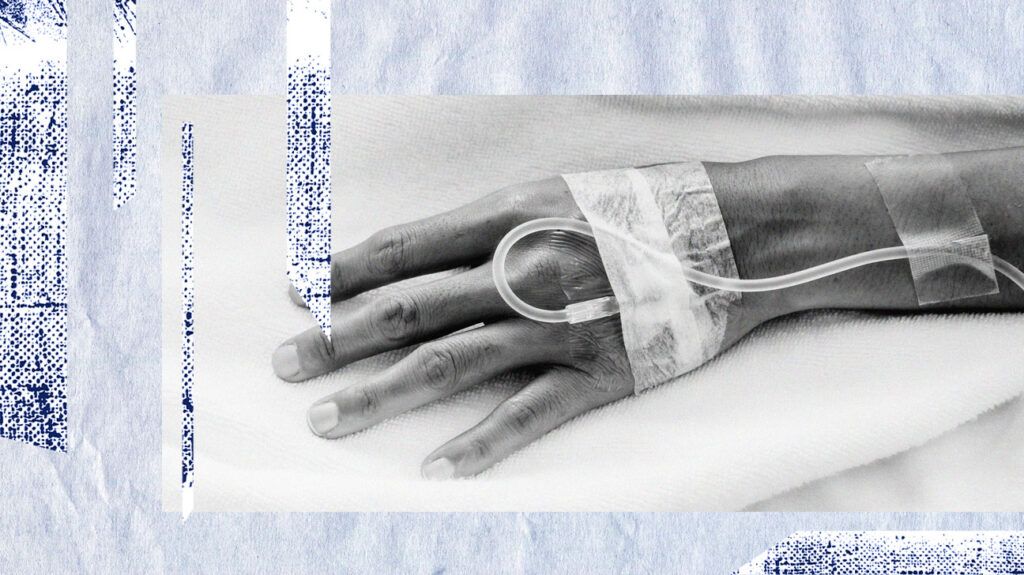
| Phlebitis | Infiltration | |
|---|---|---|
| Causes | damage to blood vessel due to IV catheter insertion | leakage of IV fluids or mediation to surrounding areas |
| Risk factors | long | large needle size and |
| Symptoms | swelling, pain, warmth, changes in skin color and texture | swelling, pain, blistering, blanching of skin, pins and needles sensation |
| Treatment | topical ointments to reduce inflammation, pain relief, hot and cold compresses | removing the IV-line, elevation, compression, and pain relief |
Phlebitis is inflammation of a vein. It can commonly occur when inserting a catheter into a vein.
The blood vessel walls can become inflamed in the area where the catheter enters. The endothelium, the cells lining the blood vessels, becomes irritated.
Causes of phlebitis
Phlebitis can occur as a common complication of using a peripheral IV catheter.
A peripheral IV catheter is a plastic tube that healthcare professionals insert into a peripheral vein to deliver medications or fluids.
Phlebitis may be
The risk of a peripheral IV catheter causing phlebitis may also include the following factors:
- site of catheter insertion
- duration of IV therapy and hospitalization
- antibiotic use
- assigned sex at birth of the person receiving treatment
- number of puncture sites, which is where the catheter enters a vein
- whether emergency intervention occurs
Symptoms of phlebitis
Symptoms of phlebitis may appear in the affected area, including:
- pain or tenderness
- swelling
- increased skin warmth
- itching
- skin discoloration
- changes to the texture of the surrounding skin, such as thickening or hardening
Treatment of phlebitis
Treatment for phlebitis may include the following:
- applying topical treatments, such as aloe vera or chamomile, to reduce swelling and inflammation
- alternating hot and cold compresses to the affected area to help reduce swelling and pain
- massaging the affected area with sesame oil
- applying marigold ointment, which has anti-inflammatory and antibacterial properties
People may require blood-thinning medications to help prevent blood clots and phlebitis from returning.
To ease symptoms of phlebitis, people can apply a warm compress, elevate the affected area when resting, and take over-the-counter pain relievers such as acetaminophen or ibuprofen.
If people are taking blood thinners, it’s important that they check with a doctor before taking ibuprofen as it may not be safe to take at the same time.
How to prevent phlebitis
According to a 2021 article, healthcare professionals may follow certain steps to help prevent phlebitis, including:
- monitoring and continuously evaluating the IV treatment
- keeping records such as dates, locations, and number of IV treatments
- removing the catheter if signs of phlebitis appear, such as warmth, redness, or tenderness
- changing a catheter and dressings as necessary
- avoiding inserting a catheter into certain areas, such as joints and wrists, as it may cause the catheter to move out of place and cause problems
- using antiseptic solutions to get rid of bacteria and other microorganisms
- maintaining proper handwashing and using gloves for carrying out procedures
Good communication between healthcare professionals and the person receiving treatment is also important. For healthcare professionals, this can include consulting the person about the location of the catheter insertion, explaining signs of phlebitis to look for, and checking whether the person experiences any discomfort or symptoms.
Infiltration is the leakage of IV medications and fluids from the insertion vein into surrounding areas.
Infiltration
Causes of infiltration
A complication of IV therapy flowing into a peripheral vein
- placement of a catheter into an area with only a small amount of soft tissue
- large needle size
- frequent insertion of a cannula
Learn more about IV injections.
The type of medication the IV delivers can also play a role in the risk of infiltration.
Symptoms of infiltration
Symptoms of infiltration may occur in the affected area and can include:
- pain
- swelling
- blistering
- blanching of the skin
- tingling, numbness, or “pins and needles” sensation
- reduction in temperature
- sensitivity at the IV insertion site
Treatment of infiltration
Healthcare professionals
- removing the IV line
- using medication such as hyaluronidase if soft tissue damage is present
- elevating the affected area
- applying mild compression to the affected area
- prescribing pain-relief medication
- monitoring for infection, which may require antibiotic treatment
Doctors will also check for complications that can occur with infiltration, such as compartment syndrome. Compartment syndrome is a buildup of pressure in the muscles.
Doctors may make referrals to surgeons — plastic or orthopedic — to treat infiltration if there is soft tissue damage or if infiltration occurs with chemotherapy.
How to prevent infiltration
According to a 2018 study, recognizing infiltration early and removing the IV may help prevent infiltration.
Frequently checking the area of the IV insertion and surrounding areas is also important, using medical grades or scales to evaluate any issues.
The person receiving treatment must understand infiltration, as this can help them recognize and report any symptoms early on.
Removing the catheter at the first signs of infiltration may help prevent inflammation from progressing and causing complications.
If people experience phlebitis symptoms while receiving IV treatment, it is important that they let a healthcare professional know.
People must contact a doctor immediately if they have the following symptoms:
- throbbing, cramping, or sudden swelling in the neck, arm, or leg
- swollen veins that feel hard or tender to touch
- pain with warm or discolored skin in the affected area
People must inform a doctor if they notice any signs of infiltration from IV therapy. A doctor may remove the IV to prevent infiltration.
Learn more about IV therapy.
Phlebitis is generally not serious and may resolve by itself within 1–2 weeks. In more severe cases, phlebitis requires treatment to help prevent blood clots or other complications.
Infiltration complications
Phlebitis is an inflammation of a vein and can be a complication of IV catheter insertion.
Infiltration can also occur as a complication of IV catheter insertion and occurs if IV fluids or medications leak into surrounding areas.
Early recognition of phlebitis or infiltration symptoms and appropriate treatment may help resolve the conditions and prevent complications.
